Chronic pain is unique in that it manages to be both predictable and unpredictable simultaneously. While long-term pain becomes familiar and unsurprising, sometimes flares of pain come on seemingly at random. It’s common to wonder, “Gee, why am I hurting so much more today?” Sometimes, flares are truly random. But often, when we look through the chaos of the flares we can see that there’s some sort of underlying pattern that precedes periods of higher pain.
Understanding these patterns is difficult, because chronic pain is so multifaceted and private that it’s sometimes hard to notice which outside factors are affecting your pain. Pain journals can be helpful tools while trying to discover what pain triggers you have; use the journal to track your daily pain, along with your daily exposure to various triggers. After a couple months, patterns should begin to emerge. Most of the triggers are unavoidable, but recognizing them is an important step in being able to engage in preemptive self-care.
While each person’s pain is fiercely individual and thus no list can be totally inclusive, there are some common pain patterns Chronic Pain sufferers might want to track.
Stress. There’s no question that stress affects how we experience pain, but the way it affects pain is not well known. For example, in cases of acute pain, induced stress (like the stress from a test) may serve as a useful distraction against pain. However, chronic pain patients have internalized, chronic stress, and the prolonged pain often makes it impossible for the body to stop producing stress hormones. This is correlated with increased pain perception and depression. It seems likely that the association between pain and stress largely depends on whether the stress is chronic or acute, as the difference of their effects on the body can be seen on a cellular level. When keeping track of stress in a pain journal, try to identify the sort of stress you’re experiencing (short-term or long-term, good or bad, etc.) as well as any other symptoms you think the stress might be exacerbating, such as mood problems, digestive issues, sleep changes, etc. If you find that stress is aggravating your pain, learning some new coping mechanisms might help you manage times of stress.
Weather. Changes in weather, particularly changes in barometric pressure, are scientifically shown to have a significant effect on pain, particularly if your pain is inflammatory in nature. As the barometric pressure drops, there’s less air-pressure around us compressing our bodily tissues, so tissues that are prone to swelling will swell. Conversely, weather systems of increasing pressure can help relieve some pain. If you notice that changes in the weather seem to accompany a change in your pain level, tracking the barometric pressure, temperature and relative humidity is a fairly thorough way to record patterns. If you’ve kept a pain journal before and would like to compare your pain levels to the weather you can do so here. Some ways to deal with weather-related pain changes are by applying compression to areas prone to swelling, keeping warm, and gentle exercise to encourage movement of fluids in the body.
Food. Food sensitivities are extremely individual, but can be an important factor in pain management. Some people might find that particular foods actually trigger a pain flare; for example, people with migraines often find that consuming MSG directly triggers an episode. Other times, it may not be noticed that a type of food causes increased pain symptoms until you eliminate it from the diet; some have found this true of things like gluten, lactose or food dye. Keeping a dietary log along with your pain journal can help clue you in on any correlations between your food intake and your pain. Always check with your doc before starting any sort of restrictive diet!
Activity. The relationship between pain levels and activity is often complex; too much or too little can cause your pain to increase. Although it often seems the intuitive response to pain, remaining sedentary can cause the body to stiffen up and muscles to lose strength, resulting in even more pain. Activity is imperative to well being when living with chronic pain because it releases feel-good endorphins , but activities that are too strenuous may cause pain to increase. By writing down what exercises and activities you preform along with your pain level, you can begin to notice what exercises leave you feeling better and which ones leave you feeling worse.
Sleep. Sleep is the time that when the body repairs itself, so it’s no surprise that sleep affects pain levels so deeply. Not all sleep is created equal; deep restorative sleep requires the sleeper passing through 5 stages of progressive relaxation. When sleep is interrupted, the body must try to start the cycle over again. If you’re tracking your sleep, some things that are beneficial to write down in the morning are: how soundly you feel you slept, how many times you woke up during the night, and how easy it was for you to fall asleep. Don’t worry too much about tracking specific times, since looking at the clock often causes anxiety over getting to sleep—totally counterproductive.
Acute Illness & Injury. One of the cruel realities of living with chronic illness is that we still have to suffer acute illnesses, too. We may describe our illness to others by saying, “Every day feels like the worst flu you’ve ever had” as a way to shed perspective on how uncomfortable we are. So when a chronically ill person experiences a terrible virus, the results are basically like getting hit by a Mac truck; incredible pain. Even minor infections can sometimes play a huge part in increasing pain and fatigue. It’s the same with acute injuries; if you experience an injury in a place that already experiences pain, it can cause your pain levels to skyrocket. Interestingly, sometimes an acute injury can help distract from chronic pain in other places. Tracking these acute problems can help explain pain fluctuations.
Sunday, December 29, 2013
Saturday, December 21, 2013
The Quiet Joints the No One Ever Knows
One of the misconceptions commonly faced by people who suffer from autoimmune arthritis is that it is exactly the same as osteoarthritis, the wear-and-tear form of arthritis which mostly affects people in old age. The fact is that autoimmune arthritis is a systemic disease which causes your autoimmune system to attack and destroy your joints; it's not known what causes it, but it certainly isn't related to wear-and-tear. The mechanism of attack is different too-- autoimmune arthritis causes blood to flood the area and cause a lot of swelling, rather than the mechanical rubbing of cartilage caused by osteoarthritis.
Something that many people don't realize about autoimmune arthritis is that it isn't picky where it will take up shop during a flare. Technically, it can affect even non-articular organs, like your heart and lungs, but it has a preference for joints. Any joint will do. Of course autoimmune arthritis affects the joints that are commonly attacked by osteoarthritis, like knees, hips, and hands, but it can also manifest itself in joints that are more exotic. It can manifest in joints most people don't know even exist.
Here are some out-of-the-way joints that can be affected by autoimmune arthritis:
Temporomandibular Joint (TMJ).
When you meet with a friend to go out for
dinner and chat, you might not realize that there's a joint working
overtime: the jaw (or TMJ). Talking, chewing and brushing your teeth
are all very basic, necessary life-tasks that require motion in your
TMJ. They all become very difficult to do when arthritis flares in these
joints. When inflammation sets in, a person can experience clicking, popping, and locking of the jaw, as well as intense pain.
Sternocostal joints.
Generally, we tend to think of our rib-cage as being a pretty solid and immobile, but there are actually several joints that help facilitate twisting, turning, and the in-and-out motions necessary for breathing. In fact, these are some of the most-used joints in the human body which never get a break from moving since we must continue breathing throughout the night, while most joints get a chance to rest. Unfortunately, it's a playground for autoimmune arthritis. Inflammation of the sternocostal joints is called Tietze Syndrome. (When inflammation isn't remarkable, the term costochondritis is often used). Sufferers experience extreme pain and difficulty breathing, wearing a bra, or moving their torsos.
Inner Ear.
Some people may be surprised to learn that our hearing is actually controlled by the motion of joints located in our ears. Very simply, the bones in our ears get hit with wavelengths from the things around us and clang together like tuning forks, vibrating noise signals into the brain. So when the joints in your ear start getting attacked by your immune system and swelling up, the tuning forks don't have room to vibrate and your hearing can run amok. Inner ear swelling can also cause tinnitus (ringing in the ears) and balance problems. This condition is sometimes referred to as Autoimmune Inner Ear Disease.
Throat.
The process of speaking takes places when we make our vocal chords vibrate together. What facilitates this vibration? You guessed it, a joint. The cricoarytenoid joint, to be specific. In a healthy throat, the cricoarytenoid joint helps make the vocal cords move up, down, and together, which is what allows us to change the pitch in our voice. When the joint is attacked by autoimmune arthritis, it inhibits these motions, and can cause hoarseness, difficulty breathing, and pain. Kelly Young has a great article about cricoarytenoid arthritis over at her website, RA Warrior.
Look at how many vital life processes, like breathing and eating, are made difficult and painful due to autoimmune arthritis.
Something that many people don't realize about autoimmune arthritis is that it isn't picky where it will take up shop during a flare. Technically, it can affect even non-articular organs, like your heart and lungs, but it has a preference for joints. Any joint will do. Of course autoimmune arthritis affects the joints that are commonly attacked by osteoarthritis, like knees, hips, and hands, but it can also manifest itself in joints that are more exotic. It can manifest in joints most people don't know even exist.
Here are some out-of-the-way joints that can be affected by autoimmune arthritis:
Temporomandibular Joint (TMJ).
 |
| Anatomy of TMJ. Source. |
Sternocostal joints.
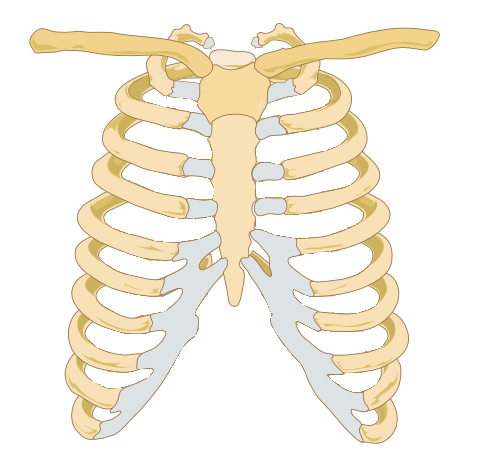 |
| Anatomy of the Rib Cage. (It swells where blue meets yellow). Source. |
Generally, we tend to think of our rib-cage as being a pretty solid and immobile, but there are actually several joints that help facilitate twisting, turning, and the in-and-out motions necessary for breathing. In fact, these are some of the most-used joints in the human body which never get a break from moving since we must continue breathing throughout the night, while most joints get a chance to rest. Unfortunately, it's a playground for autoimmune arthritis. Inflammation of the sternocostal joints is called Tietze Syndrome. (When inflammation isn't remarkable, the term costochondritis is often used). Sufferers experience extreme pain and difficulty breathing, wearing a bra, or moving their torsos.
Inner Ear.
 | |||
| Anatomy of the Human Ear. Source |
Throat.
 |
| Anatomy of the Throat. Source. |
The process of speaking takes places when we make our vocal chords vibrate together. What facilitates this vibration? You guessed it, a joint. The cricoarytenoid joint, to be specific. In a healthy throat, the cricoarytenoid joint helps make the vocal cords move up, down, and together, which is what allows us to change the pitch in our voice. When the joint is attacked by autoimmune arthritis, it inhibits these motions, and can cause hoarseness, difficulty breathing, and pain. Kelly Young has a great article about cricoarytenoid arthritis over at her website, RA Warrior.
Look at how many vital life processes, like breathing and eating, are made difficult and painful due to autoimmune arthritis.
Sunday, December 1, 2013
Silly Silver Linings
Chronic pain is an ugly, black rhinoceros of a cloud, like in Tim Burton's adaptation of Roald Dahl's, "James and the Giant Peach." Pain clouds our perspective, separates us from our loved ones, and sometimes forces us to the pits of despair. That's just what unrelenting pain is like.
Every cloud has a silver lining.
There are lots of big-ticket lessons that can be learned quicker due to dealing with chronic pain, but none of them necessarily required suffering pain to learn. Compassion, advocacy, empathy, activism... chronic pain may lead you there quicker, but there are plenty of other ways to get there too. It’s impossible for me to say that I haven’t learned a lot from my disease, but I certainly could have learned most of those things vicariously.
However, there are some things I absolutely would never have learned if not dealing with autoimmune arthritis. I never would have needed too. Silly things. Practical things. They certainly don’t make up for a life of pain, but here are some of the silver linings and lessons I never would have had without chronic pain.
1. Chronic illness makes you amazing at filling out forms. I have filled out so many forms since getting sick that I can figure out and complete almost any form like a machine. Sure, maybe there are other ways to get good at filling out forms, but by and large, healthy people don’t ever experience the variety and depth of forms that sick people do. Not only are there the medical history forms (which each doctor wants done individually, even though many medical history forms ask exactly the same question), personal symptom forms, and the corresponding insurance forms, but also a myriad of government forms if you need to utilize any public assistance. These forms then force you to familiarize yourself with all of the tax forms. There are accommodation forms if you’re physically able to work or go to school, disability forms if or when you’re not.
2. Having hand pain has taught me a million different ways to manage writing. Particularly my signature. I can give a passable signature using either hand, with my fingertip, with my fingers but without moving my hand or wrist and using my shoulders, with a pen stuck between any of my fingers, and occasionally with my right foot. I’ve learned three different types of computer dictation software, and experienced what it’s like dictating to a real person. I’ve tried non-standard keyboard configurations to try and help make typing easier (though my mind can’t escape QWERTY). Never would have tried any of these if I didn’t have to, which goes hand in hand (pun intended) with the filling out forms thing.
3. Having a cane means you always have a great resource with you. This would be even more true if you carry a sword cane, but even the standard aluminum ones (like I have) are pretty darn handy. For tasks that don’t need much dexterity, a cane easily doubles your reach—perfect for sliding things to you when you need them. It can be rolled across sore muscles for a cooling massage. It’s a great tool for stretching. It makes me feel safer knowing I could use it to defend myself. It kills spiders.
4. The health-related contents of my purse can save people in emergencies big and small. After years with no doctors really helping me, I’ve developed a compact OTC arsenal that I keep with me: Excedrin, aspirin, ibuprofen, Benadryl, antacids, etc. I always have snacks and water because they’re needed to take medication with. Also on deck are hand sanitizer, alcohol wipes and a rubber glove, because periods of being immunocompromised leave you terrified of germs. Portable hot-packs meant for outdoorsmen because they’re great for sore joints. Matches for after tummy troubles. Basically, my daily needs are what other people need in a disaster.
5. My body has become an almost entirely accurate meteorologist. It can predict fluctuations in barometric pressure and humidity with astounding precision. It always lets me know when to bring a jacket, or an umbrella. Or if an event is going to be rained out. I wish there was a way to market this knowledge to the TV meteorologists; the locals would be happier and I could use the funds!
Every cloud has a silver lining.
There are lots of big-ticket lessons that can be learned quicker due to dealing with chronic pain, but none of them necessarily required suffering pain to learn. Compassion, advocacy, empathy, activism... chronic pain may lead you there quicker, but there are plenty of other ways to get there too. It’s impossible for me to say that I haven’t learned a lot from my disease, but I certainly could have learned most of those things vicariously.
However, there are some things I absolutely would never have learned if not dealing with autoimmune arthritis. I never would have needed too. Silly things. Practical things. They certainly don’t make up for a life of pain, but here are some of the silver linings and lessons I never would have had without chronic pain.
1. Chronic illness makes you amazing at filling out forms. I have filled out so many forms since getting sick that I can figure out and complete almost any form like a machine. Sure, maybe there are other ways to get good at filling out forms, but by and large, healthy people don’t ever experience the variety and depth of forms that sick people do. Not only are there the medical history forms (which each doctor wants done individually, even though many medical history forms ask exactly the same question), personal symptom forms, and the corresponding insurance forms, but also a myriad of government forms if you need to utilize any public assistance. These forms then force you to familiarize yourself with all of the tax forms. There are accommodation forms if you’re physically able to work or go to school, disability forms if or when you’re not.
2. Having hand pain has taught me a million different ways to manage writing. Particularly my signature. I can give a passable signature using either hand, with my fingertip, with my fingers but without moving my hand or wrist and using my shoulders, with a pen stuck between any of my fingers, and occasionally with my right foot. I’ve learned three different types of computer dictation software, and experienced what it’s like dictating to a real person. I’ve tried non-standard keyboard configurations to try and help make typing easier (though my mind can’t escape QWERTY). Never would have tried any of these if I didn’t have to, which goes hand in hand (pun intended) with the filling out forms thing.
3. Having a cane means you always have a great resource with you. This would be even more true if you carry a sword cane, but even the standard aluminum ones (like I have) are pretty darn handy. For tasks that don’t need much dexterity, a cane easily doubles your reach—perfect for sliding things to you when you need them. It can be rolled across sore muscles for a cooling massage. It’s a great tool for stretching. It makes me feel safer knowing I could use it to defend myself. It kills spiders.
4. The health-related contents of my purse can save people in emergencies big and small. After years with no doctors really helping me, I’ve developed a compact OTC arsenal that I keep with me: Excedrin, aspirin, ibuprofen, Benadryl, antacids, etc. I always have snacks and water because they’re needed to take medication with. Also on deck are hand sanitizer, alcohol wipes and a rubber glove, because periods of being immunocompromised leave you terrified of germs. Portable hot-packs meant for outdoorsmen because they’re great for sore joints. Matches for after tummy troubles. Basically, my daily needs are what other people need in a disaster.
5. My body has become an almost entirely accurate meteorologist. It can predict fluctuations in barometric pressure and humidity with astounding precision. It always lets me know when to bring a jacket, or an umbrella. Or if an event is going to be rained out. I wish there was a way to market this knowledge to the TV meteorologists; the locals would be happier and I could use the funds!
Wednesday, November 27, 2013
Ambivalence, Negativity and Giving Thanks
This time of year with fellow American’s celebrating Thanksgiving, swirling around on the internet and in popular culture is the question, “What are you thankful for?” It’s an important question to ask, and practicing gratitude is a great coping mechanism. Reminding yourself of all the privilege and joy you’re thankful for on a regular basis can be a great tool towards accepting a life with chronic pain. But I’ve noticed that a problem that seems to occur this time of year: people weaponize thankfulness.
When someone is having a hard time, people might reply, “Oh, but you have so much to be thankful for,” as if it is impossible to simultaneously be thankful for what you have but remorseful at what you don’t. Others use thankfulness to launch into “inspiration porn,” saying something like, “Sally can’t get out of bed, but every day she says how thankful she is to be alive. You can get out of bed, so you should feel more thankful.” In turn, this makes people who are suffering less apt to complain and more likely in internalize future problems. It’s not uncommon to hear, “Oh, I know I shouldn’t complain, I’m lucky because of x, y, z.” This attitude disparages the lived experience of those who are suffering. I posit that there is no mutual exclusivity between being thankful and being morose, and both experiences are just as valid and worthy of discussion.
Sometimes you can be thankful and bitter about the same things. Though it’s often lost in common usage, the term “ambivalence” means the experience of holding simultaneous contradictory opinions about a particular event. Ambivalence is a common experience when living with chronic illness. When a particularly side-effect laden treatment starts to make your illness feel better, there’s a deep ambivalence between relief that the treatment is working and resentfulness that it is necessary and so toxic. Embracing this ambivalence rather than trying to quash it is a necessary step in accepting the ups and downs of life with chronic illness versus searching endlessly trying to get “back to how it was.” Ambivalence is natural and normative.
I hope that you can find lots to be thankful for this Thanksgiving, but its okay if you can’t. It’s okay to be thankful for something and mad as hell at it at the very same time. It is okay to feel all of the things you feel, irrespective of the contradiction or politically incorrectness. It’s okay to be you, where you’re at.
Wednesday, October 30, 2013
Chronic in the Kitchen
Adequate nutrition is a vital part of maintaining one's wellness. Eating well is important for everyone, but it is absolutely integral to those of us whose bodies reject the notion of "healthy"-- putting in good food is the only way to stay afloat with chronically ill bodies. We need wholesome food to take with medications so they don't screw up our stomachs and our minds. Nutrients to help protect compromised immune systems. Foods that don't make us sicker.
The problem with this is that chronic pain can make cooking feel impossible. A lot of days, it actually is impossible; you can't make a flared body go if it doesn't want to. But that doesn't negate the need for a decent meal. Fortunately, there are some things you can do when you're feeling a bit more physically capable so that flares don't leave you stranded in a food desert. I can't tell you what types of food are good for your body, but I can offer some tips that help any chronically ill would-be chef.
Bring the workspace to you with a portable table. Some kitchen designs are all about efficiency, which is great for those of us with chronic pain, but many designs make inefficient use of counter space. This translates to more walking back and forth in the kitchen as you gather your cooking implements and your ingredients-- not good when every extra step is causing pain and fatigue. Cut down on these steps around the kitchen by using a sturdy portable card-table as your cooking home-base. Place the card table close to where you'll be doing most of the food preparation-- generally near the stove. Before you start cooking, put all your needed tools and ingredients onto the card table. Now when you're cooking, you'll be able to reach behind you to grab what you need instead of having to go across the kitchen.
Use chairs to work sitting down. One of the hardest things about cooking with chronic pain is that cooking so often involves hours of standing. Standing when you chop your ingredients, standing over the stove, then standing over the sink to clean up. All this standing can be mitigated, if not eliminated, by using a chair in the kitchen. Computer chairs work great because you can adjust the height to meet the needs of each station in your kitchen. Some tasks are a little awkward in the chair-- like dishes-- but having the chair to take breaks helps keep pain levels from spiking, even if you don't complete the whole chore sitting down.
Cook huge meals and freeze individual portions. Remember when we talked about how cooking is impossible during flares? If you have leftovers in your freezer, all you have to do is pop a container into the microwave. And luckily, it's often easier to cook a bigger portion of a meal than a single serving. AllRecipes has a handy feature for its recipes which allows you to manipulate the serving size of a dish. Store (slightly cooled) leftovers in a freezer/microwave safe dish (I like glassware, but be sure not to over-fill!) There are lots of recipes out there for foods that freeze/reheat well to suit any diet plan. My personal favorite is manacotti and red-sauce; spaghetti sauce gets more flavorful as it sits, and the noodles are already cooked. Soup is also great in this regard, and you can freeze it into cute little bricks. Having a yummy, hot meal makes a flare a little more bearable.
Have the right blade. Chopping veggies is a chore that sore hands anticipate with dread. It becomes a total nightmare if you don't have a decent, sharp knife. The sharper the knife, the less pressure you have to put behind it to make it work; this translates to less pain and impact on your hands. Find out which knife type feels best to you; personally, I find that knives with bigger blades are easier because I don't have to grip as tightly. Kitchen scissors are also much easier for me to use than knives because I can rely on the pressure of two hands squeezing rather than one rocking wrist.
Break the work into chunks. To prevent yourself from getting too fatigued and sore from working in the kitchen, break your work into short, manageable stages and rest in between them. This is easier with some meals than with others, but the principal can apply to almost any meal. Take a break after getting everything together. Take a break after getting things cut up. Take a break when everything is mixed together. Do whatever you can to save your energy for when your food hits the frying-pan, when you absolutely must attend to it. When baking, you can take hours or days between some steps while you let your dough chill in the refrigerator. And don't get down on yourself for breaks- always remember it's better that something come together slowly than not at all.
Keep healthy grab-and-go food ready. There are times when you need food now. Maybe your blood sugar is crashing, maybe you need something to eat with your medication. Whatever the reason, grab-and-go food is important to keep around. Of course a lot of this depends on personal needs and taste preference, but here are some grab-and-go foods worth considering.
The problem with this is that chronic pain can make cooking feel impossible. A lot of days, it actually is impossible; you can't make a flared body go if it doesn't want to. But that doesn't negate the need for a decent meal. Fortunately, there are some things you can do when you're feeling a bit more physically capable so that flares don't leave you stranded in a food desert. I can't tell you what types of food are good for your body, but I can offer some tips that help any chronically ill would-be chef.
Bring the workspace to you with a portable table. Some kitchen designs are all about efficiency, which is great for those of us with chronic pain, but many designs make inefficient use of counter space. This translates to more walking back and forth in the kitchen as you gather your cooking implements and your ingredients-- not good when every extra step is causing pain and fatigue. Cut down on these steps around the kitchen by using a sturdy portable card-table as your cooking home-base. Place the card table close to where you'll be doing most of the food preparation-- generally near the stove. Before you start cooking, put all your needed tools and ingredients onto the card table. Now when you're cooking, you'll be able to reach behind you to grab what you need instead of having to go across the kitchen.
Use chairs to work sitting down. One of the hardest things about cooking with chronic pain is that cooking so often involves hours of standing. Standing when you chop your ingredients, standing over the stove, then standing over the sink to clean up. All this standing can be mitigated, if not eliminated, by using a chair in the kitchen. Computer chairs work great because you can adjust the height to meet the needs of each station in your kitchen. Some tasks are a little awkward in the chair-- like dishes-- but having the chair to take breaks helps keep pain levels from spiking, even if you don't complete the whole chore sitting down.
 |
| http://rejigdesign.com/11-modern-computer-chairs/ |
 |
| http://speckless.wordpress.com/2010/12/16/living-on-a-budget-1-freezing-food/ |
Have the right blade. Chopping veggies is a chore that sore hands anticipate with dread. It becomes a total nightmare if you don't have a decent, sharp knife. The sharper the knife, the less pressure you have to put behind it to make it work; this translates to less pain and impact on your hands. Find out which knife type feels best to you; personally, I find that knives with bigger blades are easier because I don't have to grip as tightly. Kitchen scissors are also much easier for me to use than knives because I can rely on the pressure of two hands squeezing rather than one rocking wrist.
 |
| http://www.bestkitchenknivesreviewed.com/best-kitchen-knife-sets |
Break the work into chunks. To prevent yourself from getting too fatigued and sore from working in the kitchen, break your work into short, manageable stages and rest in between them. This is easier with some meals than with others, but the principal can apply to almost any meal. Take a break after getting everything together. Take a break after getting things cut up. Take a break when everything is mixed together. Do whatever you can to save your energy for when your food hits the frying-pan, when you absolutely must attend to it. When baking, you can take hours or days between some steps while you let your dough chill in the refrigerator. And don't get down on yourself for breaks- always remember it's better that something come together slowly than not at all.
Keep healthy grab-and-go food ready. There are times when you need food now. Maybe your blood sugar is crashing, maybe you need something to eat with your medication. Whatever the reason, grab-and-go food is important to keep around. Of course a lot of this depends on personal needs and taste preference, but here are some grab-and-go foods worth considering.
- Almonds
- Plain yogurt with frozen fruit
- Hard-boiled eggs
- Meal-replacement bars
- Cereal
- Cheese and crackers with fruit
Monday, October 21, 2013
Life-Hacks for Chronic Pain
Life with chronic pain is hard. Pain can limit nearly every daily task one needs to accomplish in order to live a functional life. Even the little things, like showering or making food, are Olympic level tasks when faced with intense pain. Life hacking refers to any productivity trick, shortcut, skill,
or novelty method to increase productivity and efficiency, in all walks
of life. Life hacks are supposed to make the world easier-- something those of us with chronic pain can certainly appreciate. There are lots of general life hacks that can help people irrespective of disability that can be found on the web. Lifehacker and Lifehack offer a plethora of tips and tricks, as does the life-hack tag on Tumblr or Pintrest.
But for those of us with chronic pain, things that most people don't need help with become fiasco's that need their own special tips and tricks. Here are some of my favorite chronically ill life-hacks.
But for those of us with chronic pain, things that most people don't need help with become fiasco's that need their own special tips and tricks. Here are some of my favorite chronically ill life-hacks.
- Make a hobby bucket. A hobby bucket is any closed or mostly-closed container that can house the stuff you need for he projects that you like to do. It lends well to fabric and yarn craft, art supplies, scrapbooking or study-stuff, etc. Anything smallish and not super fragile that will keep you entertained. The benefit of a hobby bucket over other types of organization is that your hobby bucket is made to follow you around the house. It's closed, so it can flop over on the bed or survive that accidental fall between the couch and the desk. A bucket with a hard plastic lid makes a great tray-table to use for work space if you're someplace without a fixed surface, like in bed.
- Make warm rice buddies. Rice buddies are portable, microwavable heat-packs, and they are a godsend for sore joints and cold feet alike. They stay warm for a long time, and provide a nice moist heat, or, you can keep your rice buddy in the freezer for a cold pack that never feels so cold that it hurts like regular ice packs. They're also incredibly easy to make and to customize; it's just plain white rice (regular, not instant!) sewn inside any sort of fabric sachet. The sachet can be as simple as a plain tube-sock, or can be a beautifully patterned pillowcase. If you'd like your rice-buddy to smell like something other than white rice, you can add essential oil or tea-leaves into the rice before sewing the sachet closed. More detailed instructions available at Instructables.
- Used closed containers. Sort of in the spirit of the hobby bucket, using closed containers for everything is a great way to avoid messes, particularly if chronic pain weakens your grip or challenges your balance. Use water bottles instead of glasses or cups, and Tupperware™or another similarly locking dish instead of bowls to prevent your drink or dinner from ending up all over the floor. It's especially thrifty to save and wash the containers that come into your house already with product in them (i.e. sour cream, cool-whip, etc) Great for getting that cereal from the kitchen to the table without simultaneously getting it all over you.
- Shower Seats. Showering can be near impossible when you're battling pain and fatigue. Standing for long enough to get clean is often not an option. This is where a shower seat can save you. There are specially made shower seats available in the assistive device section of many drug-stores, or you can use any all-plastic stool you find. Put the shower seat in the shower, turn the water on, then get in and sit down-- be careful when first sitting, because your seat might slide around a bit. Now you're showering in comfort.
- Utilize opiate potentiators (with your doctor's approval). Often, good management of chronic pain involves using prescription pain medication. However, tolerance and overuse are big concerns held by doctors. One of our duties as a pain patient, then, is to work with our doctor to find the minimum amount of pain medication that we can take and still live our lives. One tool in your arsenal of using less could be the use of an opiate potentiator-- a non-narcotic substance that helps increase the effects of opiate pain medication. This is something you must talk to your doctor about before trying, but if approved, they can be used to help ameliorate your pain on very bad days. Some common potentiators are acetaminophen, caffeine and ibuprofen.
- Use speech to text. When your hands hurt, typing is frustrating at the best of times and impossible at the worst. This limits computer usage, and can leave you feeling isolated, bored and lonely. Luckily, both PC and Mac computers come with speech-to-text dictation tools right out of the box. This software allows you to speak into your computer's microphone and prompt the computer to both do commands and type for you. There's something of a learning curve as the computer learns to recognize the sounds of your unique voice, but they're pretty simple for the user from day one. Learn to access speech-to-text on your PC, or on your Mac. (If you're running Linux, you don't have an embedded dictation software, but an external product is available here.)
Wednesday, October 16, 2013
How to Live On Your Couch (And Still Feel Productive)
The unfortunate reality of many invisible illnesses is that they lay you out, flat. Pain, fatigue and other symptoms can mean a huge allotment of time can only be spent on the couch. Many illnesses cause disability to the extent that it hampers one's ability to hold a job-- the couch becomes the main resting perch as days melt into each other until the next medical appointment. Pain holds you hostage, and it's easy to let innumerable couch-locked days pass you by in a fatigued stupor. But this cycle of nothingness can breed depression, loneliness, and a feeling that you're wasting your life.
Obviously there are times when we don't need to be on the couch, and all of us with chronic pain take those days and run with them. Conversely, there are days when couch-productivity is going to be nill-- days when the pain is 9 out of 10 high and you're incoherent, there's no way you should even try to do more than exist through it. But many days, when the pain is high enough to trap you but you've still got a modicum of mental clarity, it's possible (but not always easy) to be really productive while sitting on your couch. Here are some of my favorite (thus necessarily, free) resources to help you learn, create, and better yourself from the pain-addled discomfort of your davenport.
1. That college class you always wanted to take, but never had time to fit in your schedule? Chances are, you'll be able to find it on iTunes U. From the iTunes Store menu in iTunes, there's a link for iTunes U in the upper right corner. From there, an interface introduces you to a world of totally free college lectures and courses. Many big-name universities (think MIT, Harvard, etc.) have a plethora of classes ripe for the listening. Some come with video or a PowerPoint, others are simply audio tracks. iTunes U is a great way to enrich your brain from your chair when you're not capable of much else.
2. The great Classic novels that you always felt you had an obligation to read are available from Project Gutenberg. Like their namesake, Johannes Gutenberg, father of the printing press, Project Gutenberg's aim is to help spread the written word to the masses. These eBooks are free (at least in the US) because their copyright has expired. They also offer a number of free audiobooks, read by person or by computer, if reading isn't an option for you.
3. Learn some of the peer-reviewed scientific research for your medical condition through the National Institute of Health's research database, PubMed. When you really want to go to your doctor with specific research about a symptom you're experiencing, this is the place to get it. Knowing more about your condition is empowering, but some private websites have a heavy bias and can present you with inaccurate information. The scientific community helps guard against inaccurate information by presenting studies to a large group of scientists who can all help verify the results and validity of the study. If it passes the muster, it gets put on PubMed. PubMed is also invaluable for seeing what sort of research your doctors may be involved in-- you just search their name. This can help identify what areas your doctor specializes in and often a general feel for their preconceptions about patients.
4. Become a master in retouching photos and basic graphic design with the Gimp. "Gimp" stands for GNU Image Manipulation Program, which is a long way of saying "Linux-based free photosho0p." The layout is a bit more rudimentary than the proprietary image manipulation software, but still has all the same capabilities. For those who don't know where to start, there's a plethora of websites that offer tutorials, like Gimp Tutorials and Gimpology.
5. Explore the universe through NOVA documentaries provided by PBS. There are documentaries covering a wide range of interests, all with interviews and research from top experts. Episodes are usually about an hour, and packed with good knowledge. They're fascinating, often visually stunning, and allow you to just sit back and absorb the information. Perfect for days when you need something intellectually satisfying but really can't do much at all.
P.S. Apologize for general lack of online presence. My illness has made it hard for me to do much typing. I started this post in August-- phooey on me for telling you all about productivity!
Obviously there are times when we don't need to be on the couch, and all of us with chronic pain take those days and run with them. Conversely, there are days when couch-productivity is going to be nill-- days when the pain is 9 out of 10 high and you're incoherent, there's no way you should even try to do more than exist through it. But many days, when the pain is high enough to trap you but you've still got a modicum of mental clarity, it's possible (but not always easy) to be really productive while sitting on your couch. Here are some of my favorite (thus necessarily, free) resources to help you learn, create, and better yourself from the pain-addled discomfort of your davenport.
1. That college class you always wanted to take, but never had time to fit in your schedule? Chances are, you'll be able to find it on iTunes U. From the iTunes Store menu in iTunes, there's a link for iTunes U in the upper right corner. From there, an interface introduces you to a world of totally free college lectures and courses. Many big-name universities (think MIT, Harvard, etc.) have a plethora of classes ripe for the listening. Some come with video or a PowerPoint, others are simply audio tracks. iTunes U is a great way to enrich your brain from your chair when you're not capable of much else.
2. The great Classic novels that you always felt you had an obligation to read are available from Project Gutenberg. Like their namesake, Johannes Gutenberg, father of the printing press, Project Gutenberg's aim is to help spread the written word to the masses. These eBooks are free (at least in the US) because their copyright has expired. They also offer a number of free audiobooks, read by person or by computer, if reading isn't an option for you.
3. Learn some of the peer-reviewed scientific research for your medical condition through the National Institute of Health's research database, PubMed. When you really want to go to your doctor with specific research about a symptom you're experiencing, this is the place to get it. Knowing more about your condition is empowering, but some private websites have a heavy bias and can present you with inaccurate information. The scientific community helps guard against inaccurate information by presenting studies to a large group of scientists who can all help verify the results and validity of the study. If it passes the muster, it gets put on PubMed. PubMed is also invaluable for seeing what sort of research your doctors may be involved in-- you just search their name. This can help identify what areas your doctor specializes in and often a general feel for their preconceptions about patients.
4. Become a master in retouching photos and basic graphic design with the Gimp. "Gimp" stands for GNU Image Manipulation Program, which is a long way of saying "Linux-based free photosho0p." The layout is a bit more rudimentary than the proprietary image manipulation software, but still has all the same capabilities. For those who don't know where to start, there's a plethora of websites that offer tutorials, like Gimp Tutorials and Gimpology.
5. Explore the universe through NOVA documentaries provided by PBS. There are documentaries covering a wide range of interests, all with interviews and research from top experts. Episodes are usually about an hour, and packed with good knowledge. They're fascinating, often visually stunning, and allow you to just sit back and absorb the information. Perfect for days when you need something intellectually satisfying but really can't do much at all.
P.S. Apologize for general lack of online presence. My illness has made it hard for me to do much typing. I started this post in August-- phooey on me for telling you all about productivity!
Monday, August 19, 2013
5 Things I Wish I Could Tell People About My Invisible Illness
Rheumatoid Arthritis: you don't "get it" until you get it. This is a phrase shared within the rheumatoid patient community to explain our interactions with able-bodied people. It can easily be applied to invisible illness in general; those who aren't dealing with it simply do not understand the realities of your chronically ill world. When people see brief glimpses of your disease, say on Dr. Oz or a new pharmaceutical commercial, they often believe they've gathered a true understanding and unique insights into your illness which they simply must share with you. Dealing with rheumatoid arthritis it's particularly challenging when people do not understand the difference between "wear-and-tear" osteoarthritis and inflammatory autoimmune arthritis. The former can be treated with aspirin, the latter attacks your internal organs and kills; yet people constantly confuse the two and offer rheumatoid arthritis sufferers suggestions for osteoarthritis pain.
After 7 years of living with chronic joint pain caused by autoimmune arthritis, I've learned that it's best to be as tactful as possible in dealing with people's questions, comments and concerns about my disability. Most people who offer advice or ask questions are doing so out of concern, and genuinely want me to start feeling better; they don't understand that I've answered the same questions and comments a million times before, that their anecdotal evidence isn't remotely valid as science, and that I'd really rather focus on what I can do instead of what I can't. Because most people have only the best intentions, I try to listen thoughtfully and brush people off as gently as possible, but sometimes I wish I could really tell people where to go.
In the spirit of catharsis, I figured I'd share some blunt-ass things I wish I could share with people so they could start really understanding my invisible illness.
1. If there was a diet that could cure my disease, there would be scientific proof and patients would be singing from the rooftops. Certainly there are some conditions where diet has major implications in health (gluten intolerance in those with Celiac disease, for example) but for most illnesses, there's no one specific diet that will cure you--or even help your symptoms. Usually, people try to tell me about the latest fad-diet that's made it's rounds on Dr. Oz. They talk vaguely about "inflammation" and "anti-oxidants," and make me promise I'll try the diet. Oftentimes, when I'm really desperate, I will try it, often at great personal cost, often sacrificing true nutrition. I've done extended trials with diets including: vegetarian, vegan, gluten-free, soy-free, raw-food, and fasting, and haven't noticed symptom improvement with any dietary changes. What I did notice is that life is a whole lot less fun when you're constantly concerned with what's going in your mouth. Food is one of the pleasures afforded to my crippled body, and I'm a believer that (barring allergies) no food is hurting me in moderation.
2. When I say I need to leave, it means I need to leave. Really. It doesn't mean I just need to sit down for a minute. It doesn't mean I just need a break. It shouldn't require me explaining why, exactly, it is that we need to leave. It means I need to get home now, and I need you to help me leave. Many aspects of my chronic illness aren't pretty: medications have left me with a very uneasy digestive tract, joints get filled with blood, I develop rashes... and I don't want to have to explain any of these to more people than I need to. One of the most dehumanizing aspects of chronic illness is that it strips away a person's privacy-- doctors need to know the most disgusting of physical problems, caregivers are required to help with intensely personal activities of living-- the last thing a chronically ill person needs is to lose this last bit of privacy and dignity in front of others. Our bodies require no explanation.
3. If those supplements could cure me, they'd be called "medications." Snake Oil is alive and well in the 21st Century, only today it's sold under the guise of horrifically expensive "dietary supplements" whose proponents claim treats everything from arthritis to cancer. It's incredibly presumptuous to assume that someone with a chronic illness can afford many of the outrageously priced supplements available on the market, and incredibly naive to assume that a product which has no scientific testing is somehow able to cure a life-threatening disease. My worst experience with a snake-oil salesman was actually with a Social Security Disability contracted psychologist, who insisted that my rheumatoid arthritis would be cured if I simply took these $200 a month gummy supplements, because his wife's friend's sister was "cured of her arthritis" after taking them. This guy then insisted I wasn't disabled because I was able to go to college and hadn't yet tried these supplements. Friend's moms and hairdressers have had similarly serpentine ambitions, and they are generally even harder to shake than the "try this diet" people. In reality, the FDA closely monitors the development of a medication, ensuring it's safety and efficacy; for supplements, they simply rely on the manufacturer to sell a safe product, and only step in once an unsafe supplement has entered the market and started making people sick. Similarly, they do not require supplements to list the ingredients or amount of ingredients contained within.
4. Your religion may comfort you, but please don't force it on me. People don't develop chronic illness as the result of a moral or metaphysical fault, and religious participation only helps patients who thoroughly believe it will-- much like a placebo. Forcing religious participation on those who don't want it (for example, in the form of the laying-of-hands, exorcism, or unsolicited public prayer) is tantamount to assault. Please don't ever insinuate that my chronic illness is part of your god's plan, or that it's a way to test/strengthen my faith-- these perspectives help further the belief that there's something morally defunct about people with chronic illnesses and that some moral change could make them better. This is patronizing. While I respect the rights of others to participate in any religious activity that doesn't hurt others, please don't ask me to subscribe to your dogma just because it will make you feel better. Similarly, while I always appreciate the kind thoughts associated with your prayers, they don't help me to feel any better physically, so don't expect them to. If you'd really like to understand my illness, please try talking about it to me instead of god.
5. No, I'm not too young for this cane. Canes do not have age-limits. Neither does chronic illness. My cane is a tool which helps my mobility and allows me to go places I otherwise wouldn't be able to-- that's it. It is not a fashion statement or a ploy for attention. Age and ability simply do not correlate. My cane is, frankly, none of your business.
After 7 years of living with chronic joint pain caused by autoimmune arthritis, I've learned that it's best to be as tactful as possible in dealing with people's questions, comments and concerns about my disability. Most people who offer advice or ask questions are doing so out of concern, and genuinely want me to start feeling better; they don't understand that I've answered the same questions and comments a million times before, that their anecdotal evidence isn't remotely valid as science, and that I'd really rather focus on what I can do instead of what I can't. Because most people have only the best intentions, I try to listen thoughtfully and brush people off as gently as possible, but sometimes I wish I could really tell people where to go.
In the spirit of catharsis, I figured I'd share some blunt-ass things I wish I could share with people so they could start really understanding my invisible illness.
1. If there was a diet that could cure my disease, there would be scientific proof and patients would be singing from the rooftops. Certainly there are some conditions where diet has major implications in health (gluten intolerance in those with Celiac disease, for example) but for most illnesses, there's no one specific diet that will cure you--or even help your symptoms. Usually, people try to tell me about the latest fad-diet that's made it's rounds on Dr. Oz. They talk vaguely about "inflammation" and "anti-oxidants," and make me promise I'll try the diet. Oftentimes, when I'm really desperate, I will try it, often at great personal cost, often sacrificing true nutrition. I've done extended trials with diets including: vegetarian, vegan, gluten-free, soy-free, raw-food, and fasting, and haven't noticed symptom improvement with any dietary changes. What I did notice is that life is a whole lot less fun when you're constantly concerned with what's going in your mouth. Food is one of the pleasures afforded to my crippled body, and I'm a believer that (barring allergies) no food is hurting me in moderation.
2. When I say I need to leave, it means I need to leave. Really. It doesn't mean I just need to sit down for a minute. It doesn't mean I just need a break. It shouldn't require me explaining why, exactly, it is that we need to leave. It means I need to get home now, and I need you to help me leave. Many aspects of my chronic illness aren't pretty: medications have left me with a very uneasy digestive tract, joints get filled with blood, I develop rashes... and I don't want to have to explain any of these to more people than I need to. One of the most dehumanizing aspects of chronic illness is that it strips away a person's privacy-- doctors need to know the most disgusting of physical problems, caregivers are required to help with intensely personal activities of living-- the last thing a chronically ill person needs is to lose this last bit of privacy and dignity in front of others. Our bodies require no explanation.
3. If those supplements could cure me, they'd be called "medications." Snake Oil is alive and well in the 21st Century, only today it's sold under the guise of horrifically expensive "dietary supplements" whose proponents claim treats everything from arthritis to cancer. It's incredibly presumptuous to assume that someone with a chronic illness can afford many of the outrageously priced supplements available on the market, and incredibly naive to assume that a product which has no scientific testing is somehow able to cure a life-threatening disease. My worst experience with a snake-oil salesman was actually with a Social Security Disability contracted psychologist, who insisted that my rheumatoid arthritis would be cured if I simply took these $200 a month gummy supplements, because his wife's friend's sister was "cured of her arthritis" after taking them. This guy then insisted I wasn't disabled because I was able to go to college and hadn't yet tried these supplements. Friend's moms and hairdressers have had similarly serpentine ambitions, and they are generally even harder to shake than the "try this diet" people. In reality, the FDA closely monitors the development of a medication, ensuring it's safety and efficacy; for supplements, they simply rely on the manufacturer to sell a safe product, and only step in once an unsafe supplement has entered the market and started making people sick. Similarly, they do not require supplements to list the ingredients or amount of ingredients contained within.
4. Your religion may comfort you, but please don't force it on me. People don't develop chronic illness as the result of a moral or metaphysical fault, and religious participation only helps patients who thoroughly believe it will-- much like a placebo. Forcing religious participation on those who don't want it (for example, in the form of the laying-of-hands, exorcism, or unsolicited public prayer) is tantamount to assault. Please don't ever insinuate that my chronic illness is part of your god's plan, or that it's a way to test/strengthen my faith-- these perspectives help further the belief that there's something morally defunct about people with chronic illnesses and that some moral change could make them better. This is patronizing. While I respect the rights of others to participate in any religious activity that doesn't hurt others, please don't ask me to subscribe to your dogma just because it will make you feel better. Similarly, while I always appreciate the kind thoughts associated with your prayers, they don't help me to feel any better physically, so don't expect them to. If you'd really like to understand my illness, please try talking about it to me instead of god.
5. No, I'm not too young for this cane. Canes do not have age-limits. Neither does chronic illness. My cane is a tool which helps my mobility and allows me to go places I otherwise wouldn't be able to-- that's it. It is not a fashion statement or a ploy for attention. Age and ability simply do not correlate. My cane is, frankly, none of your business.
Thursday, July 25, 2013
Disability Ethics and the Texas Filibuster
During the June 26 filibuster against Texas Senate Bill 5, senator Wendy Davis was required to stand and present about the bill's subject matter (access to abortion) for 13 hours without eating, drinking, sitting down, leaning on her podium, or going to the bathroom. The filibuster works on a "Three Strikes You're Out" policy, where if Senator Davis was found to be off topic or breaking the rules of the filibuster 3 times, she would be expelled from the floor. Twice, Senator Davis was challenged for going off topic, but one of her warnings came about when one of her colleagues-- Senator Rodney Ellis-- tried to help her tighten her back brace. Senator Tommy Williams is quoted as saying, "A filibuster is an endurance contest and it's to be made unassisted."
While Senator Davis was able to filibuster for an impressive 11+ hours, the Senate's refusal to allow her the use of an assistive device highlights an ableist paradigm in American politics. I'm interested in the discriminatory nature of the Texas filibuster process, and how it could systematically prevent people with disabilities from participating in the political process. Such overtly negative reactions to the perception of physical weakness are indicative of the internalized ableism which many don't ever think about. What does physicality have to do with politicking, really? The contents of one's character are vastly more important towards leadership than physical stamina. One of our greatest presidents, Franklin D Roosevelt, led the nation into war from a wheelchair. There's a great tradition of disabled veterans, like former senator Bob Dole, current representative James Langevin and current senator Tammy Duckworth, returning from war to enter the political sphere. Disability doesn't hinder one's performance intellectually, and in fact may cause people to pursue more intellectual ambitions once physical ones become harder to accomplish.
While Senator Davis was able to filibuster for an impressive 11+ hours, the Senate's refusal to allow her the use of an assistive device highlights an ableist paradigm in American politics. I'm interested in the discriminatory nature of the Texas filibuster process, and how it could systematically prevent people with disabilities from participating in the political process. Such overtly negative reactions to the perception of physical weakness are indicative of the internalized ableism which many don't ever think about. What does physicality have to do with politicking, really? The contents of one's character are vastly more important towards leadership than physical stamina. One of our greatest presidents, Franklin D Roosevelt, led the nation into war from a wheelchair. There's a great tradition of disabled veterans, like former senator Bob Dole, current representative James Langevin and current senator Tammy Duckworth, returning from war to enter the political sphere. Disability doesn't hinder one's performance intellectually, and in fact may cause people to pursue more intellectual ambitions once physical ones become harder to accomplish.
Monday, July 1, 2013
Disability Parking, Casual Ableism and Me
For many people, the thought of not being able to walk from the car into a business never crosses their mind. Walking is something that happens naturally for them, without pain and impairment. It's a different world for those of us with disabilities that hinder mobility. We face the daily reality of not knowing if we can make it to the grocery store and still be able to walk back to the car. When this happens enough, many of us talk to our doctors and get documentation to allow for a disabled parking placard.
Disabled parking placards are a huge boon to those of us suffering from illnesses which impact our mobility, yet for many, there's a huge stigma using one in public. The common perception is that only the elderly or those with paralysis are "worthy" of parking in disabled spaces, leaving those of us with invisible disabilities prey to the nosy eyes of other shoppers. I've received innumerable glares as I exit the car, a seemingly healthy 21 year old woman, albeit one with a cane. I've even gotten some verbal hate; one distraught man in a big-box store parking lot frantically told my driver and I that I couldn't use my tag because it was "only for wheelchairs."
In the past, I've ignored these disapproving stares and comments, but ignoring this casual ableism only allows it to continue. Here's my "action plan" for the next time I get blue-tag hate.
1. Do not feel shameful using the parking tag. The doctor agreed that it was necessary for a reason, but often I feel ashamed using my placard, and try to avoid using it in all but the biggest of parking lots. However, this often leads to an exhausting walk to and from the store which can zap away a whole day's worth of spoons. I'm learning I should feel more ashamed of harming myself by not using the tag than I should for using it. Of course I long for the day when it isn't needed anymore, but until then, it's a resource to use to my advantage.
2. Do not act shameful using the parking tag. In the past, I've avoided making eye contact with the people when I use my parking tag. It's easy to feel inferior under the icy stares, but a meek posture only helps them assume that I'm doing something wrong. Walking with a head held high helps to show I'm not ashamed of my disability and I deserve that parking spot.
3. Do not ignore the judgement. When people glare or say stupid ablist things, it's easy to just roll your eyes and brush it off, but this doesn't educate people or incite change. By engaging in a dialogue with a blue-tag hater, I can begin to pass along information about invisible illness, rheumatoid arthritis, and the necessity of not judging based on appearances. Admittedly, this is easier said than done, but I'm confident that in the future I'll be able to have a polite confrontation. (And certainly, the prednisone "roid rage" makes this easier...)
Disabled parking placards are a huge boon to those of us suffering from illnesses which impact our mobility, yet for many, there's a huge stigma using one in public. The common perception is that only the elderly or those with paralysis are "worthy" of parking in disabled spaces, leaving those of us with invisible disabilities prey to the nosy eyes of other shoppers. I've received innumerable glares as I exit the car, a seemingly healthy 21 year old woman, albeit one with a cane. I've even gotten some verbal hate; one distraught man in a big-box store parking lot frantically told my driver and I that I couldn't use my tag because it was "only for wheelchairs."
In the past, I've ignored these disapproving stares and comments, but ignoring this casual ableism only allows it to continue. Here's my "action plan" for the next time I get blue-tag hate.
1. Do not feel shameful using the parking tag. The doctor agreed that it was necessary for a reason, but often I feel ashamed using my placard, and try to avoid using it in all but the biggest of parking lots. However, this often leads to an exhausting walk to and from the store which can zap away a whole day's worth of spoons. I'm learning I should feel more ashamed of harming myself by not using the tag than I should for using it. Of course I long for the day when it isn't needed anymore, but until then, it's a resource to use to my advantage.
2. Do not act shameful using the parking tag. In the past, I've avoided making eye contact with the people when I use my parking tag. It's easy to feel inferior under the icy stares, but a meek posture only helps them assume that I'm doing something wrong. Walking with a head held high helps to show I'm not ashamed of my disability and I deserve that parking spot.
3. Do not ignore the judgement. When people glare or say stupid ablist things, it's easy to just roll your eyes and brush it off, but this doesn't educate people or incite change. By engaging in a dialogue with a blue-tag hater, I can begin to pass along information about invisible illness, rheumatoid arthritis, and the necessity of not judging based on appearances. Admittedly, this is easier said than done, but I'm confident that in the future I'll be able to have a polite confrontation. (And certainly, the prednisone "roid rage" makes this easier...)
Wednesday, June 19, 2013
Afflixerim Ergo Sum: Pain and Perception
"Cogito ergo sum: I think, therefore I am."
Descartes used this phrase when discussing his epistemology. Simply put, epistemology is the study of knowledge. Descartes was concerned with how much the human mind was actually capable of knowing. He was concerned that the mind is capable of being deceived, like it is when we're dreaming. He became convinced that there was no way of knowing whether any of our perceptions exist external to ourselves, and that ultimately the only thing a person can know irrefutably is that they exist (since there's no way to think that we don't exist, since something must be doing the thinking in the first place.) From here, Descartes posits that we know that we have perceptual experiences. We don't know the cause for these perceptual experiences (i.e. if an actual computer exists outside of you, of if you're just dreaming it up in your head) but we can't refute the fact that we experience something. So for Descartes, we're only capable of knowing two things: that we exist, and that we perceive. We're absolutely incapable of knowing anything beyond these two irrefutable facts.*
Thinking about pain within the Cartesian perspective helps take a lot of weight off my shoulders. When you understand that your perception doesn't necessarily mirror anything "in the real world" you can begin to accept your body as you feel it. As someone who has struggled for years to get a diagnosis-- I have blood-work which repeatedly shows up clear of inflammatory markers and yet have autoimmune arthritis which plagues me with pain and deformity-- it helps to understand that the act of diagnosis is intrinsically devoid of logic or merit. Whether something shows up on a piece of paper or not, the only things which I can be sure of are the things I experience: joint pain.
Afflixerim ergo sum: I hurt, therefore I am.
I've talked in the past about how to communicate with others about your pain, but it's equally important that you have internal dialogue about how your pain interacts with your perceptions and your life. Pain has a multifaceted influence on your views of the world; the way you look at a sunset, your perspectives on political issues, your viewpoint on your family. While we shouldn't feel guilty or ashamed of these interactions, understanding when and where they occur can help us frame them differently in the future. After spending the last couple weeks with pain that was MUCH higher than normal due to an injury, I've thought of several questions the chronic pain patient should ask themselves about how their perception of pain influences their life.
•Has your pain changed your outlook on life? More realistically, this question should be, "How has pain changed your outlook on life?" It's inevitable. These changes can be both positive and negative. Maybe you always used to be a cup-half-full kind of person, but find yourself looking at things in a more negative light now. Maybe you find yourself more appreciative of the small things in life now, like a nice cup of tea with a friend.
•Who do you see less now that you're in pain? Who do you see more? Why do you think that is? Pain changes relationships. It's not anybody's fault, it just happens. Recognize which people have stepped up and become more supportive, and who has fallen by the wayside. If there are relationships with people you'd like to rekindle, try to recognize why they may have deteriorated in the first place. It's a hard conversation to have with yourself, but so necessary.
•What have you learned from being in pain? I'm a firm believer that each experience we have teaches us something. Pain is no exception. Pain has taught me that I'm capable of surviving much worse than I ever would have thought possible. What has it taught you?
•When do you decide to push yourself despite the pain? When do you know it's time to rest? When dealing with chronic pain, you realize that life must go on. There are days when you have no idea how you're going to make it out of bed, and yet still manage to get yourself to that appointment, feed the kids and gas up the car. Try to identify what it is that drives you on those days, what makes those days different. Oftentimes, it's the urgency-- you can't just skip a Dr's appointment-- and it's okay if the answer is caffeine/adrenaline. It's also important to recognize that pushing yourself isn't always a good answer; it can decrease your actual efficiency and make you feel freakin' rotten. Understand when your body is telling you to rest; try and notice the signs that you're pushing yourself too far.
•Where can you go that helps lessen your pain? Distractions help lessen pain. What places distract you with their beauty, curiosity, or absurdity? Sensory distractions like soft blankets, relaxing music, and scented candles/incense help you experience things other than pain. Find what works for you.
*(Later in his writing, Descartes comes up with a cockamamie idea that we can eventually justify other sensations through the existence of a supremely powerful god... there we diverge in beliefs.)
Descartes used this phrase when discussing his epistemology. Simply put, epistemology is the study of knowledge. Descartes was concerned with how much the human mind was actually capable of knowing. He was concerned that the mind is capable of being deceived, like it is when we're dreaming. He became convinced that there was no way of knowing whether any of our perceptions exist external to ourselves, and that ultimately the only thing a person can know irrefutably is that they exist (since there's no way to think that we don't exist, since something must be doing the thinking in the first place.) From here, Descartes posits that we know that we have perceptual experiences. We don't know the cause for these perceptual experiences (i.e. if an actual computer exists outside of you, of if you're just dreaming it up in your head) but we can't refute the fact that we experience something. So for Descartes, we're only capable of knowing two things: that we exist, and that we perceive. We're absolutely incapable of knowing anything beyond these two irrefutable facts.*
Thinking about pain within the Cartesian perspective helps take a lot of weight off my shoulders. When you understand that your perception doesn't necessarily mirror anything "in the real world" you can begin to accept your body as you feel it. As someone who has struggled for years to get a diagnosis-- I have blood-work which repeatedly shows up clear of inflammatory markers and yet have autoimmune arthritis which plagues me with pain and deformity-- it helps to understand that the act of diagnosis is intrinsically devoid of logic or merit. Whether something shows up on a piece of paper or not, the only things which I can be sure of are the things I experience: joint pain.
Afflixerim ergo sum: I hurt, therefore I am.
I've talked in the past about how to communicate with others about your pain, but it's equally important that you have internal dialogue about how your pain interacts with your perceptions and your life. Pain has a multifaceted influence on your views of the world; the way you look at a sunset, your perspectives on political issues, your viewpoint on your family. While we shouldn't feel guilty or ashamed of these interactions, understanding when and where they occur can help us frame them differently in the future. After spending the last couple weeks with pain that was MUCH higher than normal due to an injury, I've thought of several questions the chronic pain patient should ask themselves about how their perception of pain influences their life.
•Has your pain changed your outlook on life? More realistically, this question should be, "How has pain changed your outlook on life?" It's inevitable. These changes can be both positive and negative. Maybe you always used to be a cup-half-full kind of person, but find yourself looking at things in a more negative light now. Maybe you find yourself more appreciative of the small things in life now, like a nice cup of tea with a friend.
•Who do you see less now that you're in pain? Who do you see more? Why do you think that is? Pain changes relationships. It's not anybody's fault, it just happens. Recognize which people have stepped up and become more supportive, and who has fallen by the wayside. If there are relationships with people you'd like to rekindle, try to recognize why they may have deteriorated in the first place. It's a hard conversation to have with yourself, but so necessary.
•What have you learned from being in pain? I'm a firm believer that each experience we have teaches us something. Pain is no exception. Pain has taught me that I'm capable of surviving much worse than I ever would have thought possible. What has it taught you?
•When do you decide to push yourself despite the pain? When do you know it's time to rest? When dealing with chronic pain, you realize that life must go on. There are days when you have no idea how you're going to make it out of bed, and yet still manage to get yourself to that appointment, feed the kids and gas up the car. Try to identify what it is that drives you on those days, what makes those days different. Oftentimes, it's the urgency-- you can't just skip a Dr's appointment-- and it's okay if the answer is caffeine/adrenaline. It's also important to recognize that pushing yourself isn't always a good answer; it can decrease your actual efficiency and make you feel freakin' rotten. Understand when your body is telling you to rest; try and notice the signs that you're pushing yourself too far.
•Where can you go that helps lessen your pain? Distractions help lessen pain. What places distract you with their beauty, curiosity, or absurdity? Sensory distractions like soft blankets, relaxing music, and scented candles/incense help you experience things other than pain. Find what works for you.
*(Later in his writing, Descartes comes up with a cockamamie idea that we can eventually justify other sensations through the existence of a supremely powerful god... there we diverge in beliefs.)
Sunday, June 2, 2013
When Side Effects Make You Crazy (Here's How To Cope)
Chronic illness equates to the use of lots of different types of medication. Try as we might to avoid them, use of prescription medication is often inevitable if we wish to preserve functioning. One of the major downfalls of prescription medication are the side effects; one glance at the sheet attached to any prescription shows innumerable complications. Most of them won't effect you, but some will.
Some of the most troubling side effects of medications are side effects which change your psychological state. Common drugs for chronic pain like prednisone, pain medication, and GABA-receptor medications all come with a slew of mental side effects, including personality change, depression, and confusion. While side effects which manifest physically can be presented efficiently to a doctor, mental changes are less clear-cut and can be missed/ignored by doctors. Physical side effects can be mitigated with complementary treatments, but doctors are often more hesitant to prescribe therapies to help mental changes. Even worse, changes to your mental state touch literally all aspects of your life; there's no way to get out of your head. Of course, the first thing to do when you experience troubling psychological side effects from a medication is to call your doctor, who can make professional assessments and alter your medication if necessary. However, if you're told to just wait them out, here are some tips for not losing your mind.
1. Journal your emotional changes. Journaling has been proven to be an extremely useful coping mechanism when dealing with stress, but the benefit here is two-fold; journals also help show if your side-effects are easing up with time (or getting worse.) Make sure to record any out-of-the ordinary feelings you're experiencing, and try to quantify how strongly you're feeling, and note if there were events which triggered the change.
2. Post-It© everything! Confusion is a huge aspect of psych. side-effects, and if you don't get control, it can ruin your life. Things like forgetting to take medication or forgetting to take dinner out of the oven can pose a serious threat to your health. For me, the GABA-receptor drugs (gabapentin and pregabalin, specifically) make me feel 6-drinks-in hammered, and consequently just as forgetful as an alcoholic. To help mitigate the confusion and forgetfulness, plastering brightly colored sticky-notes on everything helped me keep refreshing my mind. Notes showed when I'd taken my medication, which step I was on in my homework, where I'd put my cane... The bright colors really attract the eye and help highlight the important things you're doing.
3. Make sure others know what's happening. It's easy to hide when you're feeling not-yourself, but it's one of the worst times to withdraw. Letting other people know about your side-effects can have a huge protective effect: your loved ones can help look out for you, help you see changes in your personality you might miss just by self-evaluation, and help you explain your side-effects to a doctor if it becomes necessary. Similarly, letting them know about your side effects as a prophylactic effect on your relationships: everyone knows that any out-of-the-ordinary responses from you are not your fault, and remove your moral blameworthiness. I know that when I'm on prednisone, one major side effect I get is aggression, so letting those around me know beforehand that I'm going to snap helps them forgive me.
4. Cultivate some zen. The environment you put yourself in has a tremendous effect on your mental environment, so be sure to use your surroundings to your advantage. If you're dealing with "positive" psychological effects like aggression or anxiety, being in a calming surrounding with low lights and soft music can help. "Negative" psychological effects like tiredness and confusion can be remedied somewhat by maintaining adequate lighting, surrounding yourself with color, and keeping your space very tide. Music is great to help instantly make a place more zen when you can't be bothered rearranging anything else.
5. Don't blame yourself. Maybe this goes without saying, but the emotions you feel as a result of medication are not your fault, and you're not responsible. The only thing you can control are your physical responses to the mental state. It's easy to feel like a crummy person when you're snapping at your loved ones, forgetful, or depressed, but these things are beyond your control, and they will pass. Take lots of deep breaths, and learn to forgive yourself. You can get through this.
6. Talk to someone, and know when things have become an emergency. A lot of medications have warnings about increased suicide risk, and this is a very real, deadly concern. It's important that you have someone to talk to about any feelings you might be having, but particularly about any suicidal ideation. Your doctor or a therapist are great people to have conversations about your mental health with, so is a responsible loved one or your patient advocate. If you need someone to speak to immediately, call 911. Alternately, here's an international list of suicide-hotlines. If you're feeling like killing yourself, or if any of your psychological side-effects are life-threatening, please get help.
Some of the most troubling side effects of medications are side effects which change your psychological state. Common drugs for chronic pain like prednisone, pain medication, and GABA-receptor medications all come with a slew of mental side effects, including personality change, depression, and confusion. While side effects which manifest physically can be presented efficiently to a doctor, mental changes are less clear-cut and can be missed/ignored by doctors. Physical side effects can be mitigated with complementary treatments, but doctors are often more hesitant to prescribe therapies to help mental changes. Even worse, changes to your mental state touch literally all aspects of your life; there's no way to get out of your head. Of course, the first thing to do when you experience troubling psychological side effects from a medication is to call your doctor, who can make professional assessments and alter your medication if necessary. However, if you're told to just wait them out, here are some tips for not losing your mind.
1. Journal your emotional changes. Journaling has been proven to be an extremely useful coping mechanism when dealing with stress, but the benefit here is two-fold; journals also help show if your side-effects are easing up with time (or getting worse.) Make sure to record any out-of-the ordinary feelings you're experiencing, and try to quantify how strongly you're feeling, and note if there were events which triggered the change.
2. Post-It© everything! Confusion is a huge aspect of psych. side-effects, and if you don't get control, it can ruin your life. Things like forgetting to take medication or forgetting to take dinner out of the oven can pose a serious threat to your health. For me, the GABA-receptor drugs (gabapentin and pregabalin, specifically) make me feel 6-drinks-in hammered, and consequently just as forgetful as an alcoholic. To help mitigate the confusion and forgetfulness, plastering brightly colored sticky-notes on everything helped me keep refreshing my mind. Notes showed when I'd taken my medication, which step I was on in my homework, where I'd put my cane... The bright colors really attract the eye and help highlight the important things you're doing.
3. Make sure others know what's happening. It's easy to hide when you're feeling not-yourself, but it's one of the worst times to withdraw. Letting other people know about your side-effects can have a huge protective effect: your loved ones can help look out for you, help you see changes in your personality you might miss just by self-evaluation, and help you explain your side-effects to a doctor if it becomes necessary. Similarly, letting them know about your side effects as a prophylactic effect on your relationships: everyone knows that any out-of-the-ordinary responses from you are not your fault, and remove your moral blameworthiness. I know that when I'm on prednisone, one major side effect I get is aggression, so letting those around me know beforehand that I'm going to snap helps them forgive me.
4. Cultivate some zen. The environment you put yourself in has a tremendous effect on your mental environment, so be sure to use your surroundings to your advantage. If you're dealing with "positive" psychological effects like aggression or anxiety, being in a calming surrounding with low lights and soft music can help. "Negative" psychological effects like tiredness and confusion can be remedied somewhat by maintaining adequate lighting, surrounding yourself with color, and keeping your space very tide. Music is great to help instantly make a place more zen when you can't be bothered rearranging anything else.
5. Don't blame yourself. Maybe this goes without saying, but the emotions you feel as a result of medication are not your fault, and you're not responsible. The only thing you can control are your physical responses to the mental state. It's easy to feel like a crummy person when you're snapping at your loved ones, forgetful, or depressed, but these things are beyond your control, and they will pass. Take lots of deep breaths, and learn to forgive yourself. You can get through this.
6. Talk to someone, and know when things have become an emergency. A lot of medications have warnings about increased suicide risk, and this is a very real, deadly concern. It's important that you have someone to talk to about any feelings you might be having, but particularly about any suicidal ideation. Your doctor or a therapist are great people to have conversations about your mental health with, so is a responsible loved one or your patient advocate. If you need someone to speak to immediately, call 911. Alternately, here's an international list of suicide-hotlines. If you're feeling like killing yourself, or if any of your psychological side-effects are life-threatening, please get help.
Friday, May 31, 2013
Tracking Your Pain: How to Effectively Communicate Your Pain Symptoms
After 8 years of chronic pain, I consider myself something of a pain-connoisseur. I've tasted the nectar of throbbing joints, whiffed the bouquet of stabbing stomach pains, and drank in all manner of aching awfulness. During those years, I've learned that while our pain may be subjective, a good description can help explain your situation to medical professionals and avoid miscommunications. Maintaining a consistent way of describing your pain can be a great way to assess how well a new treatment may be working, or showing any trends in your illness.
So how do you explain your pain symptoms to your doctor? One of the best ways is through the use of a pain journal where you enter information about your pain at some general times every day (ie morning-afternoon-evening) Here are some basic things to keep track of in your pain journal to help explain your pain to a medical professional.
1. When noting pain's intensity, start on the same playing field, and start on a good one. Pain is one of the most subjective experiences in the world. To try and quantify pain in a more objective way, medical professionals usually use a standard "pain chart." My doctor's office has the standard Wong-Baker smiley-face 10-point chart for pain.
A quick look shows you that it makes absolutely no sense. If it hurts a little, why is he smiling? Does #4 look pained, or puzzled? And certainly, my face doesn't always read like a little smushed up ball even when the pain is "hurts a whole lot" intense. If my doctor and I are even playing on the same playing-field with this chart... the playing field stinks. I find the more objective Mankoski Pain Scale has a more accurate description of what my "pain level" actually feels like. I keep a copy on the back of my pain-journal, and make sure I print one off for each doctor to keep as well.
3. Record the location of your pain (and use tech to help!) Knowing where the pain is is tantamount to diagnosis on your doctor's part. One way to really show doctors what's hurting is to take a photo of yourself (or find a photo of a basic anatomical illustration) and shade in the parts that are causing pain. Shade in areas of intense pain more darkly. If the pain is radiating, use arrows to show which way it travels. Note whether the pain is superficial (near the skin) or deep inside.
4. Be cognizant of what makes your pain change. Pains respond differently to the daily wear we put our bodies through. Noticing how the changes in your day effect your pain can help pinpoint it's cause. Does your pain get better or worse with activity? Does your stress level correlate with your pain? Do certain activities like climbing stairs or reaching overhead aggravate your pain? Do things like showers, stretching, or a full night's sleep makes your pain level decrease? More broadly, notice if there certain weather patterns that correlate with better or worse pain.If your pain lets up at certain points, note the duration of time when you're in pain, and the duration of time you're pain free.
5. Make your pain human by relating it to your life. Pain is such an abstract concept that it's often easier for doctors to think in terms of what's concrete, and the way your pain interferes with your life is a concrete measure. If you're having trouble with tasks of daily living like doing laundry, climbing stairs, or personal grooming, make note of that. If it's interfering with your family life or your work responsibilities, mention how.
So how do you explain your pain symptoms to your doctor? One of the best ways is through the use of a pain journal where you enter information about your pain at some general times every day (ie morning-afternoon-evening) Here are some basic things to keep track of in your pain journal to help explain your pain to a medical professional.
1. When noting pain's intensity, start on the same playing field, and start on a good one. Pain is one of the most subjective experiences in the world. To try and quantify pain in a more objective way, medical professionals usually use a standard "pain chart." My doctor's office has the standard Wong-Baker smiley-face 10-point chart for pain.
A quick look shows you that it makes absolutely no sense. If it hurts a little, why is he smiling? Does #4 look pained, or puzzled? And certainly, my face doesn't always read like a little smushed up ball even when the pain is "hurts a whole lot" intense. If my doctor and I are even playing on the same playing-field with this chart... the playing field stinks. I find the more objective Mankoski Pain Scale has a more accurate description of what my "pain level" actually feels like. I keep a copy on the back of my pain-journal, and make sure I print one off for each doctor to keep as well.
- 0 - Pain Free
- 1 - Very minor annoyance - occasional minor twinges.
- 2 - Minor Annoyance - occasional strong twinges.
- 3 - Annoying enough to be distracting
- 4 - Can be ignored if you are really involved in your work, but still distracting
- 5 - Can't be ignored for more than 30 minutes.
- 6 - Can't be ignored for any length of time, but you can still go to work and participate in social activities.
- 7 - Makes it difficult to concentrate, interferes with sleep. You can still function with effort.
- 8 - Physical activity severely limited. You can read and converse with effort. Nausea and dizziness set in as factors of pain.
- 9 - Unable to speak. Crying out or moaning uncontrollably - near delirium.
- 10 - Unconscious. Pain makes you pass out.
- © Andrea Mankoski
3. Record the location of your pain (and use tech to help!) Knowing where the pain is is tantamount to diagnosis on your doctor's part. One way to really show doctors what's hurting is to take a photo of yourself (or find a photo of a basic anatomical illustration) and shade in the parts that are causing pain. Shade in areas of intense pain more darkly. If the pain is radiating, use arrows to show which way it travels. Note whether the pain is superficial (near the skin) or deep inside.
4. Be cognizant of what makes your pain change. Pains respond differently to the daily wear we put our bodies through. Noticing how the changes in your day effect your pain can help pinpoint it's cause. Does your pain get better or worse with activity? Does your stress level correlate with your pain? Do certain activities like climbing stairs or reaching overhead aggravate your pain? Do things like showers, stretching, or a full night's sleep makes your pain level decrease? More broadly, notice if there certain weather patterns that correlate with better or worse pain.If your pain lets up at certain points, note the duration of time when you're in pain, and the duration of time you're pain free.
5. Make your pain human by relating it to your life. Pain is such an abstract concept that it's often easier for doctors to think in terms of what's concrete, and the way your pain interferes with your life is a concrete measure. If you're having trouble with tasks of daily living like doing laundry, climbing stairs, or personal grooming, make note of that. If it's interfering with your family life or your work responsibilities, mention how.
Friday, May 24, 2013
Communication Breakdown: Tips for Fighting Through The Telephone Jungle
When acquaintances ask me what I do, I often say that having a chronic illness is a full-time job. Unfortunately, part of that full-time job is hours upon hours spent talking on the telephone while attempting to navigate our bureaucratic medical system and arrange care. Month after month, the phone bill shows more time spent trying to make appointments with doctors than time spent chatting with friends. And sometimes talking on the telephone can be a very flawed system for relaying information. As you get patched back and forth to receptionists, nurses, and other office staff, information can be missed or misheard, and it can have an impact on your health care outcome.
Recently, I had a misunderstanding with the nurse at my doctors office; she didn't ask/seem interested in my pain level, and upon finding out that my MRI was negative for avascular necrosis, promptly canceled my follow-up appointment because she figured there was nothing wrong. It got figured out in the end, but the miscommunication caused a lot of stress, and also got me thinking about specific protocol to follow to make sure nothing like this happens again.
1. Find our who you're talking to. This is a must-know in case you have any trouble after your phone call. Most hospitals have a fairly good policy in place for staff giving their name and job-position when on the phone, but if you come across someone who doesn't offer their name, don't be afraid to ask. Ask for a name every time you get patched through to someone new, and right the names down if you're prone to forgetting. That way, f you need to call back you can ask for the people that you talked to previously, follow up with any questions, or file a report if something is handled unprofessionally.
2. Take notes. If you recieve an unexpected call from the doctor's office, it's not unreasonable to ask them to give you a second to grab a note pad. Jotting down notes about what you're told as well as what your replies are helps stimulate a more productive conversation. You'll know when you haven't mentioned something, remember the information relayed to you, and can use your notes to gather your thoughts as the conversation progresses. Also, keeping a pen and paper handy helps guard against forgetting what date and time any future appointments may be.
3. Go high-tech... Be a spy! Many phones have features which allow the owner to record voice conversations, and I'm a huge proponent. Recording a conversation keeps both parties honest-- and like taking notes, recording allows you to go back and process. The caveat is that some states require you to notify others when you're recording, so if you live in one of these states, make sure to notify the person you're talking with.
4. Check back. If you have a conversation that leaves you confused or upset, call back or visit the office. That way, you can confirm any instructions, ask all the questions you might have, and air any grievances or concerns you may have. If nobody knows that you're not on the same page, problems unfortunately will go ignored. We must be our own advocates, because there's nobody else to straighten things out.
5. Know when to give up and talk to someone else. Some people are... bitchy. There, I said it. Some people are mean or ignorant or generally rotten, and they do not deserve the stress they'll impose on you. If you keep talking to one person and are having many miscommunications, or feel belittled or ignored, stay calm and politely ask to talk to somebody else, or try calling back a different day. Because our emotional affect is blunted on the phone, tempers can flare quickly. Because it's your health on the line, you have every right to request somebody else. Difficulty with language barriers, accents, and enunciation can also be reasons to ask for someone else. Bottom line is, they are running a business, while you are running your life.
Recently, I had a misunderstanding with the nurse at my doctors office; she didn't ask/seem interested in my pain level, and upon finding out that my MRI was negative for avascular necrosis, promptly canceled my follow-up appointment because she figured there was nothing wrong. It got figured out in the end, but the miscommunication caused a lot of stress, and also got me thinking about specific protocol to follow to make sure nothing like this happens again.
1. Find our who you're talking to. This is a must-know in case you have any trouble after your phone call. Most hospitals have a fairly good policy in place for staff giving their name and job-position when on the phone, but if you come across someone who doesn't offer their name, don't be afraid to ask. Ask for a name every time you get patched through to someone new, and right the names down if you're prone to forgetting. That way, f you need to call back you can ask for the people that you talked to previously, follow up with any questions, or file a report if something is handled unprofessionally.
2. Take notes. If you recieve an unexpected call from the doctor's office, it's not unreasonable to ask them to give you a second to grab a note pad. Jotting down notes about what you're told as well as what your replies are helps stimulate a more productive conversation. You'll know when you haven't mentioned something, remember the information relayed to you, and can use your notes to gather your thoughts as the conversation progresses. Also, keeping a pen and paper handy helps guard against forgetting what date and time any future appointments may be.
3. Go high-tech... Be a spy! Many phones have features which allow the owner to record voice conversations, and I'm a huge proponent. Recording a conversation keeps both parties honest-- and like taking notes, recording allows you to go back and process. The caveat is that some states require you to notify others when you're recording, so if you live in one of these states, make sure to notify the person you're talking with.
4. Check back. If you have a conversation that leaves you confused or upset, call back or visit the office. That way, you can confirm any instructions, ask all the questions you might have, and air any grievances or concerns you may have. If nobody knows that you're not on the same page, problems unfortunately will go ignored. We must be our own advocates, because there's nobody else to straighten things out.
5. Know when to give up and talk to someone else. Some people are... bitchy. There, I said it. Some people are mean or ignorant or generally rotten, and they do not deserve the stress they'll impose on you. If you keep talking to one person and are having many miscommunications, or feel belittled or ignored, stay calm and politely ask to talk to somebody else, or try calling back a different day. Because our emotional affect is blunted on the phone, tempers can flare quickly. Because it's your health on the line, you have every right to request somebody else. Difficulty with language barriers, accents, and enunciation can also be reasons to ask for someone else. Bottom line is, they are running a business, while you are running your life.
Tuesday, May 14, 2013
The Pros and Cons of Dr. Google
Ahh, Dr. Google, the one doc who still makes house-class, no symptom too insignificant to warrant careful consideration. One click, and all your symptoms are run through a myriad of databases capable of telling you virtually anything and everything that might be going wrong. But should you Google those symptoms?
I injured my hip in aquatic physical therapy over 2 months ago, and it hasn't healed. X-Rays haven't revealed any dislocation or fracture, and my doctor recently suggested a remote possibility of avascular necrosis of the hip. He explained that, basically, it means that your bone is damaged and isn't getting enough blood, so it stops building up. I left that office that day with a choice to make: do I go to the net and look it up? There are pros and cons to using the great resource that is the hospital of the World Wide Web; here are a few that I've thought about.
Pro's and Con's of Dr. Google
Pro: Knowledge can help you achieve a better differential diagnosis. A differential diagnosis is the list of all possible diagnoses that might be causing the symptoms you're experiencing within a reasonable doubt. If you go online and look up a diagnosis that's been suggested and it sounds totally off-base, you can help your doctor eliminate it from your differential diagnosis. If Dr. Google leads to a disease that fits your symptoms well, you could talk to your doctor about that disease. Bottom line, sometimes a little extra knowledge is helpful in communication with your doctor.
Con: Knowledge can freak you out. There are a ton of horror stories online about missed diagnoses, treatments that backfired, horrible prognoses from illnesses, and general medical malady, and they can drag you down. I'm not one of those people who emphasizes the role of mindfulness and chronic illness, but I believe that a negative, terrified attitude can only make a poor health situation even worse, and it's hard to filter out all the negative information online. A good case in point are drug side-effects: many effects happen to only a handful of people on the medication, but reading them may scare you away from trying it. An adage to remember is: what has been seen cannot be unseen.
Pro: Internet research can help you feel proactive. When you're ill, the world starts circling around you in ways that are completely out of your control. Symptoms go un-managed, and it can take months to get in to see a doctor to figure out the problem. Turning to the internet gives you something to do in the meantime, and sometimes advice on new home-remedies to try (or those to stay away from.) It's proven that a feeling of control helps people cope better with challenging situations, and using the internet helps you feel more in control.
Con: Not everything you read is true. Does that really need to be said? But when you're hurting, it's easy to latch on to the hope of some miracle diet or new restorative snake-oil, and it's easy to get exploited. Some people share information that is blatantly false, knowingly or not. And moreover, not everything you read on the internet is true for you. Just because something on the internet has convincing results doesn't mean it will work for your specific situation. Just because a diagnosis sounds convincing doesn't mean it's what you have. A hefty dose of skepticism is always necessary.
Pro: The devil you know is better than the devil you don't. For me, after years of undiagnosed chronic illness, this is always what keeps me looking, motivated, curious. It's more comforting for me to do a lot of research and be able to prepare myself for a number of different things going wrong than to know something isn't right with my body but choose to ignore it. This is a personal choice. For me, the agony of not knowing outweighs the agony of preparing for the worst.
I injured my hip in aquatic physical therapy over 2 months ago, and it hasn't healed. X-Rays haven't revealed any dislocation or fracture, and my doctor recently suggested a remote possibility of avascular necrosis of the hip. He explained that, basically, it means that your bone is damaged and isn't getting enough blood, so it stops building up. I left that office that day with a choice to make: do I go to the net and look it up? There are pros and cons to using the great resource that is the hospital of the World Wide Web; here are a few that I've thought about.
Pro's and Con's of Dr. Google
Pro: Knowledge can help you achieve a better differential diagnosis. A differential diagnosis is the list of all possible diagnoses that might be causing the symptoms you're experiencing within a reasonable doubt. If you go online and look up a diagnosis that's been suggested and it sounds totally off-base, you can help your doctor eliminate it from your differential diagnosis. If Dr. Google leads to a disease that fits your symptoms well, you could talk to your doctor about that disease. Bottom line, sometimes a little extra knowledge is helpful in communication with your doctor.
Con: Knowledge can freak you out. There are a ton of horror stories online about missed diagnoses, treatments that backfired, horrible prognoses from illnesses, and general medical malady, and they can drag you down. I'm not one of those people who emphasizes the role of mindfulness and chronic illness, but I believe that a negative, terrified attitude can only make a poor health situation even worse, and it's hard to filter out all the negative information online. A good case in point are drug side-effects: many effects happen to only a handful of people on the medication, but reading them may scare you away from trying it. An adage to remember is: what has been seen cannot be unseen.
Pro: Internet research can help you feel proactive. When you're ill, the world starts circling around you in ways that are completely out of your control. Symptoms go un-managed, and it can take months to get in to see a doctor to figure out the problem. Turning to the internet gives you something to do in the meantime, and sometimes advice on new home-remedies to try (or those to stay away from.) It's proven that a feeling of control helps people cope better with challenging situations, and using the internet helps you feel more in control.
Con: Not everything you read is true. Does that really need to be said? But when you're hurting, it's easy to latch on to the hope of some miracle diet or new restorative snake-oil, and it's easy to get exploited. Some people share information that is blatantly false, knowingly or not. And moreover, not everything you read on the internet is true for you. Just because something on the internet has convincing results doesn't mean it will work for your specific situation. Just because a diagnosis sounds convincing doesn't mean it's what you have. A hefty dose of skepticism is always necessary.
Pro: The devil you know is better than the devil you don't. For me, after years of undiagnosed chronic illness, this is always what keeps me looking, motivated, curious. It's more comforting for me to do a lot of research and be able to prepare myself for a number of different things going wrong than to know something isn't right with my body but choose to ignore it. This is a personal choice. For me, the agony of not knowing outweighs the agony of preparing for the worst.
Saturday, May 4, 2013
Chronic Pain Fashion Part 2: Fabrics That Aren't Evil
In my last post about chronic pain fashion, I talked about ditching the pants. But another integral step of comfortable clothing when you feel like crap is finding the type of fabric that makes you feel best. Fabrics that cling too tight and squeeze, itch, or don't breathe can make you feel even more awful when you're flaring; some can even promote symptoms like rashes and fevers. he best way to try out a variety of fabric is to go to the local secondhand store; wool, silk, cashmere and other luxurious fabrics become affordable, but you can also run your hands over a lot of polyester crap and figure out what that feels like too.A lot of this is about personal choice and trying stuff out for you, but here are some tips I've learned about various fabrics.
Cotton: Cotton is my standby fabric because it's so versatile. It breathes really well, which is a huge concern for those of us who suffer autoimmune fevers and hot swollen joints. It doesn't cling, it drapes well across the body and it moves with you-- important when you've got limited range of motion or when you use mobility devices. There are a bunch of different types of weave pattern for cotton from see-through-beach-cover-up to chunky-sweater, but essentially the clothes made of cotton are fairly lightweight and soft to the touch, so it's a great fabric for all manners of layering. The only drawback I've found is that cotton shrinks.
Wool: For outer-wear, wool is excellent. It's super warm, but it still breathes. For that reason, it's really great for layering. Being cold makes my joint pain and stiffness worse, an wool is excellent for keeping me toasty but not making me roast. Wool's a little stiffer than cotton, but overall still has excellent movement. The one downside can be that wool can be itchy. Really itchy. This is combated by either buying brushed wool (hello, cashmere!), or by strategic placement of layers between you and the wool. For this reason, many things made out of wool come lined in silk. Speaking of which...
Silk: Not much trumps the luxury factor of silk, and treating yourself to garments made out of such a soft material is a great pick-me-up for days when your illness leaves you feeling like crap. Silk blouses and scarves are soft and flowey, great for if you're dealing with skin issues, or if you just want to be cozy with something soft. Silk dresses and nighties are also wonderful, as both make you feel like you're wearing nothing.
Man-Mades (aka, polyester, nylon, lycra, etc.): Ahh, the dreaded petroleum! I try to stay away from man made fibers as much as I can, for a few reasons: it doesn't breathe, it clings all wrong, and it doesn't allow for good body-temperature regulation, which can leave you feeling like crap. Unfortunately, it's is really hard to avoid. As a general rule, a little can be okay, but you don't want it to make up the bulk of your garment.
Cotton: Cotton is my standby fabric because it's so versatile. It breathes really well, which is a huge concern for those of us who suffer autoimmune fevers and hot swollen joints. It doesn't cling, it drapes well across the body and it moves with you-- important when you've got limited range of motion or when you use mobility devices. There are a bunch of different types of weave pattern for cotton from see-through-beach-cover-up to chunky-sweater, but essentially the clothes made of cotton are fairly lightweight and soft to the touch, so it's a great fabric for all manners of layering. The only drawback I've found is that cotton shrinks.
Wool: For outer-wear, wool is excellent. It's super warm, but it still breathes. For that reason, it's really great for layering. Being cold makes my joint pain and stiffness worse, an wool is excellent for keeping me toasty but not making me roast. Wool's a little stiffer than cotton, but overall still has excellent movement. The one downside can be that wool can be itchy. Really itchy. This is combated by either buying brushed wool (hello, cashmere!), or by strategic placement of layers between you and the wool. For this reason, many things made out of wool come lined in silk. Speaking of which...
Silk: Not much trumps the luxury factor of silk, and treating yourself to garments made out of such a soft material is a great pick-me-up for days when your illness leaves you feeling like crap. Silk blouses and scarves are soft and flowey, great for if you're dealing with skin issues, or if you just want to be cozy with something soft. Silk dresses and nighties are also wonderful, as both make you feel like you're wearing nothing.
Man-Mades (aka, polyester, nylon, lycra, etc.): Ahh, the dreaded petroleum! I try to stay away from man made fibers as much as I can, for a few reasons: it doesn't breathe, it clings all wrong, and it doesn't allow for good body-temperature regulation, which can leave you feeling like crap. Unfortunately, it's is really hard to avoid. As a general rule, a little can be okay, but you don't want it to make up the bulk of your garment.
Sunday, April 28, 2013
You Are Not Alone: The Importance of Finding a Patient Community
As a chronic illness patient, it's easy to feel alone in your circumstances. Navigating the medical community is arduous at best, terrifying at worst, and sometimes it seems that there couldn't be a person in the world who understands what you're going through. The reality is that there are a whole lot of people who are dealing with the same things, and when things are really bad it's important to have a community to fall back on to show you it couldn't be further from the truth. Having people to gripe to, to ask advice from, and to share camaraderie with helps remove some of the fear and depression innate in any chronic illness.
These communities exist in many different forms. They are certainly not one-size-fits-all. There are a myriad of disease specific communities, and communities for disease in general. Here are some places you might find your community.
These communities exist in many different forms. They are certainly not one-size-fits-all. There are a myriad of disease specific communities, and communities for disease in general. Here are some places you might find your community.
- DailyStrength. DailyStrength (called DS by it's users) has a multitude of support groups for all different illnesses, as well as for interpersonal problems ranging from loneliness to divorce. I've mentioned this site before, and I'll mention it again, because I've found it to be a wonderful place to get support and ask questions.
- Hospital-Facilitated Support Groups: Many healthcare organizations run patient-to-patient support groups face-to-face a couple times a month. Most places have things like cancer and dialysis support; finding a chronic pain support group might be a bit more difficult, but certainly not impossible. Most hospitals keep listings of support groups on their websites; the local newspaper is another place to look.
- Awareness activities: Organizations hold events to promote awareness for various conditions, and if you're able to attend it's a great place to meet other people suffering the same thing. This type of event is much easier to attend if you live in a larger area, but sometimes they pop up in small towns too. The Americaan Chronic Pain Association's calendar tracks chronic pain events, here's a schedule for Arthritis Walks by state.
- Social Media: If just the idea of going the an arthritis walk makes your knees ache, social media is another viable way to connect with other people in the chronic illness community. Twitter, Tumblr, Facebook... all have huge amounts of followers, and many accounts held by people with chronic illness. Searching tags is often the best way to find these groups; once found, suss them out of a few days to make sure it's the type of community you'd like to be involved in and have your name/handle attached to.
Thursday, April 25, 2013
Chronic Pain Fashion, Part 1; Ditching the Pants
When you're dealing with joint pain (and tummy issues from medication) like me, the vast majority of pants are hell. Jeans are particularly foul culprits; hard to pull on, painful to zip and button, and either too constricting or always falling down. Unfortunately, pants are now ubiquitous in our society. So what are some other options? Dresses, skirts, and the elusive pair of pants that doesn't suck. Here are some tips on each.
*I don't have personal experience with the articles of clothing pictured above, just with similar clothes. It's up to you to try it on and find out if it's comfortable for you or not!
- Dresses. Flow-y and loose, dresses are a great wardrobe choice when dealing with chronic pain, because good ones essentially feel like wearing nothing. I like ones with some elastic that you can either step into or pull over. Cotton or jersey are breathable and don't put much pressure on your body in the way some synthetic materials do. They allow free movement, most don't have any fasteners to deal with, and they look super classy. Unfortunately, they're not great in colder weather, harder to get on when your arms are painful and stiff, and bad for high-wind.
 |
| Found here |
 |
| Found here |
- Skirts. The trick to finding the right skirt is to find a great fit and a nice material. I usually avoid any fasteners other than snaps to be easy on my hands. Skirts are a viable option for winter if they're long enough and made of the right stuff; wool is warm and comfy if you wear tights or leggings under to protect from itchiness. Good for when you can't get your arms above your head
 |
| Found here |
 |
| Found here |
- Alternative Pants. I know, it sounds counter-intuitive to the blog title, but not all pants are evil, and there are times when skirts and dresses simply aren't appropriate. One major time when I don't want to be caught with any sort of bare leg is dusk in Mosquito Country. Pants are required. The key to good pants are movement, softness of material, and fastener type.You want something that flexes with your body, rather than doing anything to constrain it.One design that keeps this in mind is the yoga-pant. Yoga pants are built for maximum comfort, and usually just slide right on without any fastening. They come in a variety of prints, and some actually look pretty classy. They also make your butt look fantastic. Cotton dress pants are another good alternative. I look for them in the mens section, since the sizing there actually makes sense and they're usually cheaper than ladies dress pants. Snaps and hooks are good fasteners.
 |
| Found here |
 |
| Found here |
*I don't have personal experience with the articles of clothing pictured above, just with similar clothes. It's up to you to try it on and find out if it's comfortable for you or not!
Subscribe to:
Posts (Atom)